Osgood Schlatter’s and Sinding-Larsen Disease
Typical Symptoms
Osgood Schlatter’s (OSD) and Sinding-Larsen (SLD) are similar problems at opposing ends of the patella tendon at the front of the knee. They both cause pain, which can limit activity, sometimes there can be swelling and with OSD there can also be hardening of the tissue to leave a hard bony lump.
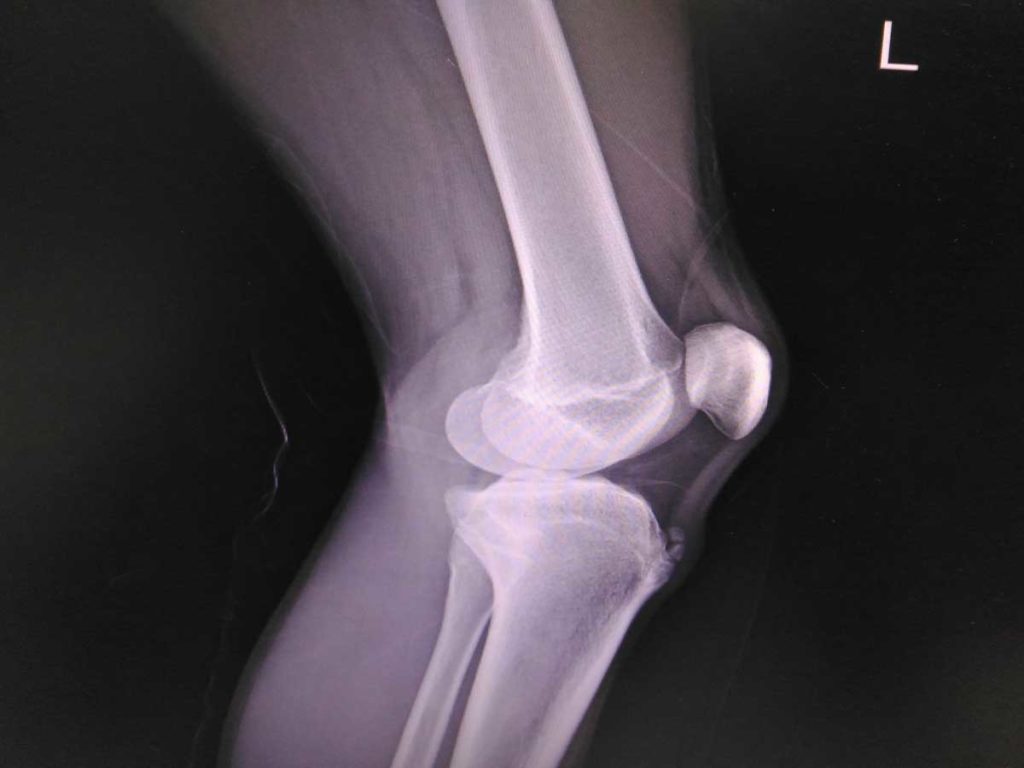
What causes it?
Both tend to occur in young, physically active individuals who usually have a training or competition load beyond what they can physically manage. Often, this might be due to an upcoming event, a change in training schedule or event the individual themselves adding in extra training.
OSD tends to occur at the distal (far) end of the tendon and the latter, SLD, occurs proximally (near top).
How can I help myself?
It is useful to think back to when the symptoms began and what the contributing / aggravating factors might be. Offloading from training is important but complete rest is usually unnecessary. Collaboration between coaches, parents and athletes is important to manage this effectively. Tightness in muscles can be improved with stretching and perhaps seeing a sports therapist.
If there is swelling and redness around the tendon, simple PRICE measures can help reduce this and pain can be improved with pain-killers such as anti-inflammatories.
When to seek help?
If your symptoms are ongoing despite trying to offload from activity and taking measures to reduce pain, and it is impacting your function, then you should be assessed as soon as possible.
What are the treatment options?
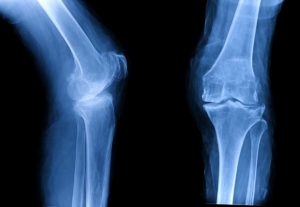
Your clinician will assess you with a thorough history and examination. They may organise an X-ray to look for calcific (hardening) changes in the tendon or perform an ultrasound scan to assess the patella tendon and identify if there is any smaller calcifications or tears in it.
In addition to managing load, working with a physiotherapist is recommended to look at specific exercises and a gait analysis, with a podiatrist, and help identify if running pattern is a contributing factor.
In some situations, shockwave therapy may be helpful for pain symptoms and most cases will settle with these measures. On occasion, further imaging with an MRI scan will be requested to identify any smaller changes in the tendon, but surgical intervention is not usually required.